Climate Remains a Question in Zika Virus Spread
The Wellcome Trust just published a Q&A with Columbia University/IRI’s Madeleine Thomson in which she explains the relationship between Zika and climate, as well her outlook for future epidemics and the role of climate science, excerpted in part below.
How are Zika virus and the climate related?
We know that virtually all vector-borne diseases have a climate dimension. Temperature drives the rate at which vectors and pathogens [things that cause disease, such as viruses and bacteria] develop, while rainfall often supports the creation of sites for the vectors to breed.
A lot of work has already been done on the relationship between dengue and climate, looking at rainfall and temperature and at how El Niño and La Niña have an impact. The vectors for dengue are Aedes aegypti and Aedes albopictus mosquitoes. This is a starting point for Zika, as it shares the same vectors. A. aegypti is an urban mosquito that breeds in containers where fresh water might collect, from flower vases to water drums to broken coconut shells. It is found only in tropical and subtropical regions. A. albopictus has the potential for a slightly broader geographic range as its eggs can survive long periods in a dormant state.
How easy is it to predict what and where the next big epidemic will be?
The recent expansion of the A. aegypti and A. albopictus mosquitoes is very much associated with globalisation – things like the movement of shipping containers around the world, air travel, population movement, forest clearing and urbanisation.
We have to expect more of this type of emergence: new diseases that were historically isolated (and therefore didn’t have a big impact) which can spread very rapidly and have a huge impact on a large community. Zika is not the last. There’ll be others, but predicting exactly what, where and when is really difficult. Instead we need to prepare ourselves to be able to respond rapidly to a broad range of possible threats.
How can climate scientists help the world prepare better for future epidemics?
Climate scientists have to be interested in how their science can benefit society in a practical way. Then they have to really look at the timeframe of decisions. Climate variability, which includes the impact of El Niño and La Niña, has a significant short-term impact on global temperatures and regional rainfall. Longer-term trends in climate (including those associated with human-induced changes) interact with this variability, meaning that, while likely changes in 50 or 100 years’ time are well-understood for some regions, making predictions for the next 5 to 15 years is very difficult. And this is the timeframe often requested by decision makers.
People are often asked questions around climate change, but if you are down in the weeds as a malaria, dengue or Zika control person, you are really largely dealing in the timeframe of climate variability. What is happening now? What happened last year? What might happen next year in this particular locality? However, policy makers still need to be aware of what the longer-term trends might be so they can build the institutional capacity needed to respond effectively down the line. You need climate scientists who are able to support decision makers across a range of time and spatial scales.
What’s the one change you’d make in the world to make us better prepared for epidemics?
I would incorporate some fairly straightforward information on climate and environmental disease drivers in all epidemiological training that happens around the world. Outbreak response people can work with partners in countries to get the best data, but if the health sector doesn’t understand the issues, particularly around climate variability and change, then it’s very hard for them to use the information effectively.
Read the full text and a Spanish translation of the interview here on the Wellcome Trust blog.
This week, the Pan American Health Organization is hosting a meeting in Washington, DC, to consult with experts about the Zika virus. Attendees will discuss the implications of the virus on public health as well as priorities for Zika research going forward.
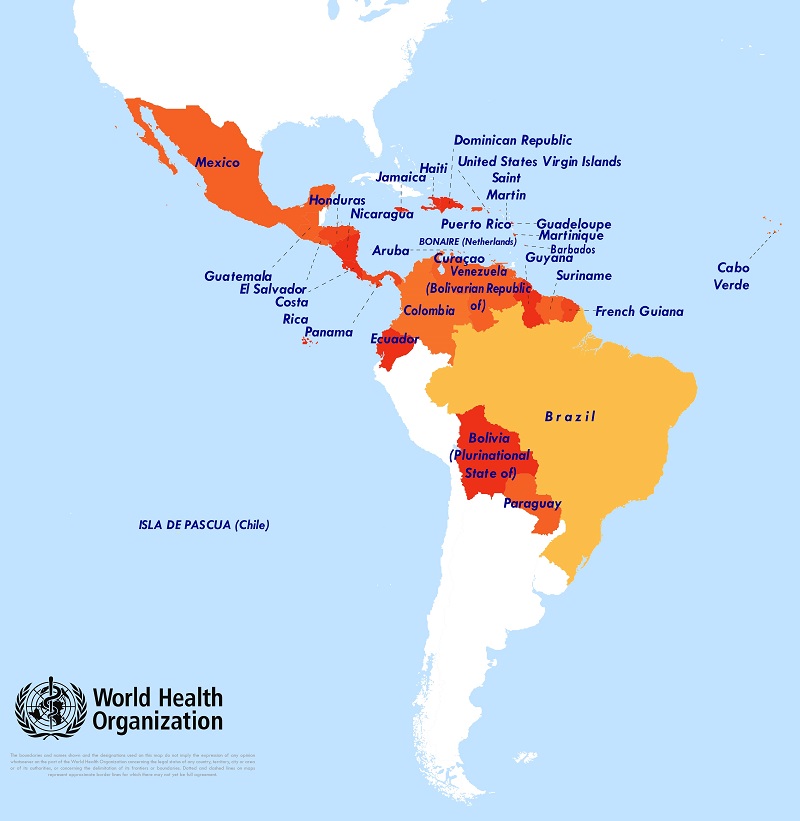
Countries and territories with autochthonous of Zika virus circulation 2007-2016. Source: PAHO.
The influence of climate and weather on the virus is an important component. Thomson, a senior research scientist at the International Research Institute for Climate and Society, will be among those attending. IRI is a PAHO/WHO Collaborating Centre on Early Warning Systems for Malaria and other Climate Sensitive Diseases, which Thomson directs. Also attending the meeting is Ángel Muñoz, a recent Columbia University doctoral graduate and adjunct researcher at IRI, who is currently a postdoctoral research associate at NOAA’s Geophysical Fluid Dynamics Laboratory.
Thomson and Muñoz will be lending their expertise based on previous research and application of that research, including that of dengue fever, which is transmitted via the same mosquito as Zika.

You must be logged in to post a comment.